Malawi’s ban on dual practice divides health sector
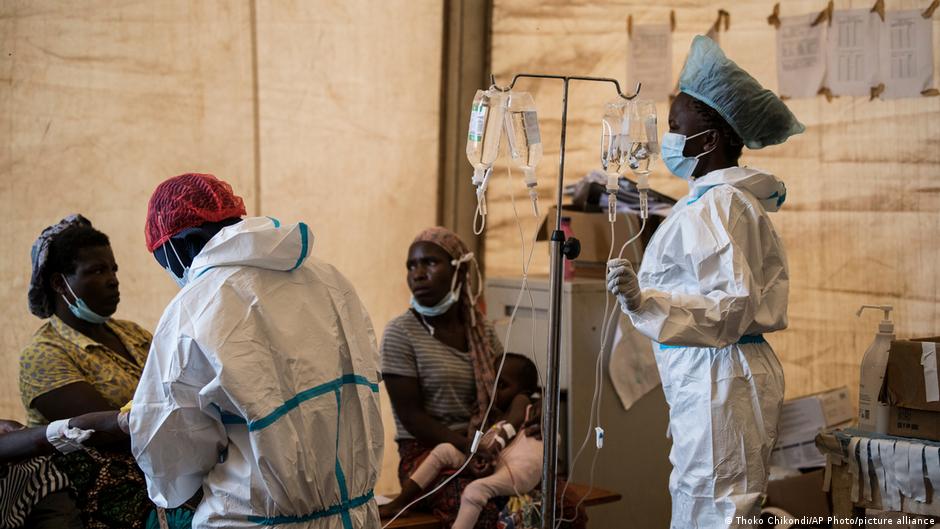
Malawi’s Ban on Dual Practice Sparks Debate in Health Sector
Malawi has implemented a prohibition on dual practice, preventing public health workers from maintaining private medical roles. While the government asserts this measure combats corruption, medical professionals express concerns it may exacerbate staffing shortages. The policy, enforced last month, restricts public-sector doctors and nurses from working in private clinics, hospitals, pharmacies, or diagnostic centers while still employed by the state. It further mandates that any worker owning or partially owning a private facility must relinquish their stake within 30 days or face termination and legal consequences.
The directive emerged after an investigative report by the Nyasa Times exposed a widespread corruption network in multiple public hospitals. Patients were often compelled to pay unlawful fees for services meant to be free. Undercover investigations revealed how security guards, clerks, nurses, and clinicians collaborated in bribery schemes, enabling some to bypass queues while others endured delays or missed care. This system effectively turned access to treatment into a cash-dependent process, disadvantaging poorer patients across various facilities.
Presidential Rationale
Malawi’s president, Peter Mutharika, defended the ban as necessary to address longstanding abuses tied to dual practice. He highlighted how some public hospital staff demanded informal payments, redirected patients to their private clinics, and even diverted medicines from government hospitals for resale in private pharmacies. Reports also pointed to frequent absences of health workers from their public posts to attend to private patients, creating critical service gaps in already strained institutions.
Industry Pushback
Health experts argue the policy lacks foundation and violates human rights. Maziko Matemba, executive director of the Health and Rights Education Program, told DW,
“I think the directive has no basis. It is illegal and an infringement of human rights.”
Low public-sector wages have pushed many doctors and nurses to take private jobs to meet financial needs. Specialists fear the ban could drive them to abandon public service entirely, worsening an existing crisis in hospital staffing.
Matemba also warned the policy might hinder medical innovation.
“One of the issues coming out is that the medical community foresees a future that lacks innovation, because ownership or running private clinics goes a long way toward improving health services in the country,”
he said. The Society of Medical Doctors in Malawi has begun planning a legal challenge, claiming the directive is overly strict and risks destabilizing the national health system.
Public Support and Criticism
Despite industry pushback, some Malawians welcome the ban. A resident interviewed by DW noted,
“The directive is quite okay because here in Malawi we’ve seen that sometimes you go to a public hospital and there is no medication. They refer you to a certain hospital or pharmacy.”
DW’s report in Lilongwe revealed that most pharmacies to which patients are referred are owned by the same health workers.
Supporters, including the Malawi Health Equity Network, view the measure as a “long-overdue intervention” to shield citizens from illegal fees, coercion, and unequal care access. They argue it is a vital step in curbing corruption and upholding ethical standards in public hospitals. However, critics like Solomon Chomba, chairperson of the Human Resource for Health Coalition, say the approach is “wrong” and undermines economic rights, warning of potential resignations as health workers resist closing private ventures.
